Best Medical Alert Systems of 2026
After ranking the equipment, response times, fall detection and mobile options of 30 medical alert systems, Bay Alarm Medical wound up on top due to its 30-second or less response times.

SafeHome.org may receive compensation from some providers listed on this page. Learn More
We may receive compensation from some providers listed on this page. Learn More
Best Overall

Bay Alarm Medical offers both high quality technology and products, with rapid response and service. Their cellular system with GPS is the best on the market and they’re the only company offering an in-car monitoring solution.
Best Fall Detection

Medical Guardian offers a high-end product suite at above average prices. The company has an A+ BBB rating and thousands of positive customer reviews. Recently they’ve developed a smart watch with advanced monitoring capabilities.
Best Security Company Offering

ADT Health keeps things simple with three plans to choose from. Their mobile units come with GPS location tracking with optional fall detection. We just wish the device was more discreet, but otherwise ADT Health makes the grade.
Best Overall

Best Fall Detection

Best Security Company Offering

We’ve spent years testing and evaluating medical alert systems, and in 2026, the landscape continues to evolve with smarter, more reliable devices. Our team focuses on real-world performance, ease of use, and responsive monitoring – because when it comes to personal safety, every second counts. After rigorous hands-on testing, research into manufacturer reliability, and in-home trials, our top picks are Bay Alarm, Medical Guardian, and ADT Medical.
Our recommendations come from experience. We’ve worn the devices, tested the monitoring services, and compared features, battery life, and connectivity under real-world conditions. Whether you need a system for yourself or a loved one, you’ll find this year’s best medical alert systems for different uses below. Keep reading.
| System |
Bay Alarm Medical

|
Medical Guardian

|
ADT Medical Alert System

|
MobileHelp

|
Lifeline

|
Medical Alert

|
LifeFone

|
GetSafe

|
Lively

|
Aloe Care Health

|
|---|---|---|---|---|---|---|---|---|---|---|
| Ranking |
1st

|
2nd

|
3rd

|
4th

|
5th

|
6th

|
7th

|
8th

|
9th

|
10th

|
| SecureScore™ | 9.3 | 9.1 | 8.9 | 8.7 | 8.2 | 8.3 | 8.4 | 7.9 | 7.8 | 8.6 |
| Best Accolade | Best Overall | Best Fall Detection | Best Security Offering | Best Range | Best Brand Recognition | Best Response Center | Best Customer Service | Best In-Home | Best Mobile Options | Best for Caregivers |
| Monthly Cost | Starting at $27.95/mo | Starting at $27.95/mo | Starting at $31.99/mo | Starting at $24.95/mo | Starting at $27.95/mo | Starting at $27.95/mo | Starting at $24.95/mo | Starting at $29.95/mo | Starting at $24.99/mo | Starting at $39.99/mo |
| Warranty | Lifetime | Yes (optional protection plan available) | Lifetime | Yes | 1-Year | Lifetime | Lifetime | 1-Year | None | Yes |
| Read Review | Bay Alarm Medical Review | Medical Guardian Review | Lively Review |

Bay Alarm Medical offers a full lineup of in-home and mobile medical alert systems, including a standalone medical alert smartwatch that works without pairing to a phone. What sets them apart for us is the combination of affordable pricing and a track record that stretches back over 75 years. Their monitoring centers even carry TMA Five Diamond Certification, which is the gold standard in emergency response.
Bay Alarm Medical’s packages deliver what we look for in a medical alert system: strong protection and fair pricing. They offer everything from straightforward at-home systems with free equipment to advanced smartwatch options, and their cellular devices run on Verizon or AT&T for broader coverage. We also like their app. With an active monitoring plan and a mobile device, caregivers can check GPS location, update contacts, and manage account details directly from their phones.
Bay Alarm Medical backs every device with TMA Five Diamond Certified monitoring. Monitoring starts at $27.95 per month, which is on par with competitors. Here’s a current breakdown of what each package includes and costs.
| Bay Alarm Medical Equipment | What’s in the Box | Equipment Price | Monthly Monitoring Price |
|---|---|---|---|
| SOS Home |
|
Free | $27.95 – $44.95 |
| SOS All-In-One |
|
$149 – $247 | $34.95 – $54.95 |
| SOS Micro |
|
$149 | $34.95 – $59.95 |
| SOS Smartwatch |
|
$199 | $39.95 – $64.95 |
FYI: Bay Alarm Medical regularly runs sales events, with discounts up to 50 percent off equipment packages. Sometimes, you’ll also get free shipping and a free month of monitoring. Looking for more ways to save? Check out our list of the best affordable medical alert systems.
| Connectivity | Landline and cellular |
|---|---|
| Fall Detection | $10/month |
| In-home Range | Up to 1,000 feet |
| Battery Backup | Up to 32 hours |
| GPS Option | Yes |
| Money-back Guarantee | 15-day |

Medical Guardian combines cutting-edge innovation with budget-friendly pricing. Their product range includes advanced options like medical alert smartwatches and feature-rich mobile apps. Still, they maintain competitive rates without locking customers into restrictive long-term contracts. This approach makes quality medical alert protection available to a wide range of users.
Medical Guardian doesn’t lock users into long-term contracts, which we consider a major advantage. You can try the service for a single month, and if it’s not a fit, you’re only paying for that first month of monitoring.
We’ve also seen strong performance from their equipment. In our tests, the in-home wearable buttons stayed connected from up to 1,400 feet away. That’s far enough to cover large yards or gardens without dropping protection.
Medical Guardian offers multiple systems and monitoring plans, making it simple to find the right fit for your daily routine. For those who spend most of their time at home, the MGHome landline or cellular system is ideal. The landline offers free equipment, with monthly monitoring starting at $27.95. For the cellular version, you’ll pay $149.95 for equipment with monitoring starting at $34.95 per month.
For more active lifestyles, their mobile devices — MGMini, MGMini Lite, and MGMove — deliver protection wherever you go. Monthly monitoring ranges from $38.95 to $46.95, and all three models feature GPS, Wi-Fi, and 4G LTE connectivity. With unlimited range, you maintain full coverage both at home and on the go, no matter where life takes you.
| Connectivity | Landline, cellular, and Wi-fi |
|---|---|
| Fall Detection | $10/month |
| In-home Range | Up to 1,400 feet |
| Battery Backup | Up to 36 hours |
| GPS Option | Yes |
| Money-back Guarantee | None |

We know ADT as one of the top home security systems. While their medical alert systems lack the high-tech capabilities of their security systems, they deliver the same quality monitoring backed by over 150 years of industry experience. ADT runs their own UL-certified monitoring centers for their medical alert systems, ensuring consistent, professional emergency response.
ADT has earned its reputation as one of the strongest home security brands in the U.S. With more than 150 years in the industry, they’ve had plenty of time to refine how they protect customers.
ADT Medical Alert keeps its lineup straightforward with three plans: Medical Alert Basic (in-home, landline), Medical Alert Plus (cellular with optional fall detection), and On-The-Go (mobile). Monthly costs for ADT Medical Alert range from $31.99 to $41.99 with optional add-ons that can increase the rate further. However, equipment comes free with a subscription and $99 activation fee.
As expected from a long-standing provider, ADT prioritizes customer service and reliability. Their ForeveRate price lock guarantee means you’ll never see an increase in your monitoring rate. All plans also come with no long-term contracts, transparent pricing, and lifetime equipment warranties, giving users flexibility and peace of mind.
Expert Insight: If you already have ADT home security, ask about bundling medical alert services for a discount. Some customers reduce their activation fee by combining services.
| Connectivity | Landline or Cellular |
|---|---|
| Fall Detection | $11/month |
| In-home Range | 300 feet or 600 feet, depending on system |
| Battery Backup | Up to 20 hours |
| GPS Option | Yes |
| Money-back Guarantee | 30-day |

As the name implies, MobileHelp built its reputation on mobile medical alert devices. They still offer some of the most compact GPS-enabled mobile devices on the market, with their smallest unit easily fitting into a pocket. Now, they also offer in-home systems with an impressive range. For the best of both worlds, you can bundle mobile and in-home systems for a discounted price with MobileHelp's Duo system.
MobileHelp doesn’t offer as many options as Bay Alarm or Medical Guardian. They only offer two mobile devices and two in-home devices. Still, these systems offer all the key features you’d expect from any medical alert system — and then some — at an affordable price point.
As long as you’re in an area with an AT&T signal, MobileHelp’s mobile devices work anywhere you go. That keeps seniors safe without impacting their freedom. Best of all, MobileHelp Micro monitoring costs $34.95 per month, which includes free coverage for a spouse. We think this is good value if there are two people in the household who need protection.
The in-home Classic Cellular package includes a help button with the farthest range in the industry of up to 1,400 feet. Pricing starts at $24.95 per month. Want both mobile and at-home coverage? The Home Duo Bundle gets you there for $44.95 a month.
FYI: While MobileHelp’s equipment may not have the sleekest modern designs compared to other medical alert systems on this list, they offer exceptional reliability and some of the most budget-friendly medical alert options available today.
| Connectivity | Landline or Cellular |
|---|---|
| Fall Detection | $5.50/month |
| In-home Range | Up to 1,400 feet |
| Battery Backup | Up to 30 hours |
| GPS Option | Yes |
| Money-back Guarantee | None |

Lifeline is among the most recognizable names in the medical alert system industry. That’s no accident. The company provides solid equipment and reliable monitoring. Plus, it’s one of the few medical alert companies out there that includes bonus features like fall detection in its base packages. Sooner or later, most seniors need the security of a fall detection plan, and it’s nice when companies provide it at no extra cost.
Lifeline is one of the pioneers of the medical alert industry. Originally, it provided services to hospitals and other health care facilities, but for a number of years now, its primary business has been medical alert systems for the general public. Its hallmark is providing quality equipment and reliable monitoring for an affordable price.
Lifeline offers three plan options: two at-home plans and one on-the-go plan. Pricing starts at $29.95 per month and goes up to $39.95 per month. A one-time activation fee applies with each at-home plan, which covers the cost of equipment.
In fact, Lifeline’s prices include many features and extras you pay for separately with other companies. A lockbox for emergency services, for instance, comes with all systems if you sign up for an annual plan. So, even though LifeLine’s prices are higher than some competitors, you’re getting features that those competitors charge extra for.
| Connectivity | Landline or Cellular |
|---|---|
| Fall Detection | $15/month |
| In-home Range | Up to 800 feet |
| Battery Backup | Up to 30 hours |
| GPS Option | Yes |
| Money-back Guarantee | None |

Medical Alert makes medical alert systems affordable enough for virtually every senior with rates starting at $19.95 per month. All annual plans come with the equipment, too, so your only upfront cost will be for monitoring. Despite those low costs, Medical Alert still provides great service with some of the fastest response times in the industry.
Medical Alert monitoring plans start at $19.95, one of the lowest prices in the market. They charge more for their mobile systems — $34.95 a month. Both plans include rented equipment as well. There’s also no hidden fees or long-term contracts to worry about. That means you can return your Medical Alert system anytime with no penalties.
For Medical Alert’s smartwatches, there’s a one-time upfront cost of $159 for the device itself. It delivers emergency assistance anywhere you go, with built-in GPS tracking, a heart rate monitor, and voice command options. The monthly monitoring fee starts at $34.95.
FYI: Medical Alert has redundant CSAA Five Diamond Certified response centers that offer 24/7 monitoring and bilingual operators in 140 different languages.
Whichever system you choose, all Medical Alert devices are easy to set up and use. In-home systems just need to be plugged in and activated. On-the-go systems need to be charged and activated. Then, press the help button anytime you need assistance and a trained operator will be on the line.
| Connectivity | Landline and cellular |
|---|---|
| Fall Detection | $10/month |
| In-home Range | Up to 800 feet |
| Battery Backup | Up to 30 hours |
| GPS Option | Yes |
| Money-back Guarantee | 30-day |

While LifeFone offers home-based medical alert systems, we recommend their on-the-go systems. Mobile protection is what they do best. In fact, LifeFone offers four mobile systems, including a smart watch option, so it’s easy to find a package that fits your lifestyle.
When it comes to mobile medical alert systems, no other company on this list offers as many options as LifeFone. All of their mobile systems feature quality, water resistant equipment and long-lasting batteries lasting up to 10 days. The only exception is the Safe Watch’s 24-hour battery life, but it comes with unique features like a weather app, GPS locator, and heart monitor.
LifeFone’s in-home systems come with free equipment, and monitoring starts at just $24.95 per month. These devices include built-in temperature sensors and a 1,300-foot range.
On-the-go monitoring plans range from $37.95 to $43.95 per month. Fall detection is only $5 per month extra, roughly half of what most competitors charge. Plus, all plans are available on a month-to-month basis with no long-term contracts required.
| Connectivity | Landline or cellular |
|---|---|
| Fall Detection | $5/month |
| In-home Range | Up to 1,300 feet |
| GPS Option | Yes |
| Money-back Guarantee | 30-day |


GetSafe offers a unique medical alert system that does not require a wearable device — no lanyards, wrist devices, or buttons of any kind. Instead, they install listening devices around your home that work through voice commands. Of course, you can add a wearable device, if you want, and GetSafe makes sure to position panic buttons around your home as a failsafe. That’s the type of reliability we expect from a company owned by Bay Alarm, our favorite medical alert system.
There is something freeing about being able to take off the wearables and wander around your home without a tether. And we were impressed by just how responsive the system is to voice commands. For instance, if you say “Call 9-1-1” these high-tech devices immediately notify emergency personnel.
Unlike most at-home systems, GetSafe uses 4G LTE cellular connectivity rather than Wi-Fi, making it more reliable and allowing the system to keep working even during a power outage. They also include two-way talk for easy communication with caregivers.
The main downside is upfront costs. GetSafe charges $79 for their base station, which includes only one wall unit. Monitoring starts at $29.95 per month, with fall detection available as an add-on for an extra $10 per month.
| Connectivity | Cellular |
|---|---|
| Fall Detection | $10/month |
| In-home Range | Up to 1,300 feet |
| Battery Backup | Up to 32 hours |
| GPS Option | No |
| Money-back Guarantee | 30-day |

Lively offers mobile medical alert systems in the form of a pendant, cell phone, or smartphone. Their monitoring is also unique, with the option for a care advocate and an on-call nurse you can ask health-related questions.
Lively began life as a phone company aimed at seniors. It was only natural that it would branch out into medical alert monitoring as well. The unique element of Lively’s phone service is that you can combine it with medical protection without the need for buying a separate device. The phone itself – either a Jitterbug Smart3 or a Jitterbug Flip2 – works as the monitor, but you can also text, email, check the news, and order from Amazon just like you would with any other smartphone. A cellphone is far less conspicuous than a wearable button. One bill helps de-clutter your life.
If you’re looking for a more traditional approach to medical alert coverage, though, Lively recently introduced an emergency button you can wear on a lanyard. For some seniors, a button can be far safer since it’s easier to use. Rather than fumbling with a lot of buttons, you simply summon help with a single push. These devices still make use of cell phone technology. Your phone serves as your system base, so you have the freedom to go anywhere in the world.
Lively is a well-known name with a great reputation when it comes to senior products and services. Lively’s traditional medical alert devices offer monitoring plans starting at $24.99 per month that include features such as a 24/7 hotline for help, the Lively Link app for family alerts, product replacement, and fall detection, depending on the package you choose. They have a wide variety of affordable accessories you can purchase as well. And, if you are in need of a mobile phone, they offer flip-phones and smartphones with a 5Star emergency button and other advanced features like brain games and voice typing.
Savings Alert: Keep an eye out for Lively deals. In the past, they’ve slashed prices by up to 50 percent on devices like the Mobile2 push button device. The company has even run two-for-one deals on its product range and included several months of discounted monitoring with new plan sign-ups.
| Connectivity | Cellular and Wi-Fi |
|---|---|
| Fall Detection | $9.99 per month |
| In-home Range | N/A |
| Battery Backup | Up to 40 hours |
| GPS Option | Yes |
| Money-back Guarantee | 30-day |

Aloe Care Health bills itself as the world’s most advanced medical alert system, and we won’t disagree. Aloe systems are far more than just an emergency button connected to a monitoring center. Devices come equipped with environmental sensors, for instance, and can be operated using just your voice. Of course, Aloe Care Health is a bit more expensive than other systems on this list. After all, you get what you pay for. And honestly, these systems can be a little more than most seniors need. If you or a loved one has special needs, though, Aloe Care Health may be exactly the medical alert system you’re looking for.
The key to the Aloe Health system is a mix of monitors that work together to keep seniors safe. The heart of the system is a hub that allows users to contact health care services in two different ways – with the touch of a button or via their voices. The hub also includes built in motion, temperature, and air quality sensors providing an additional layer of health protection. Plus, users have a wearable button they can use to summon help if they’re away from the hub.
Perhaps the most unique aspect of the Aloe Health system, though, is the way it allows caregivers to stay constantly updated on their loved ones’ health. Checking in on how your senior is doing is as easy as touching a button. The secure Aloe Health app provides real-time information gathered from the hub’s sensors and trend insights based on this data. Plus, it allows for one-touch talk any time.
In addition, Aloe Health offers a number of high-tech add-ons like a sleep mat that analyzes sleep patterns and a radar fall detection device. The company continues to develop new products and promotes its system as one that can adapt and expand to meet changing individual needs.
In terms of packages, you can choose from several options, including mobile systems and at-home packages featuring an advanced base unit. Aloe Care Health prices start at $39.99 per month for basic monitoring and range up to $59.99 monthly for the comprehensive Essentials Plus plan with mobile and at-home coverage. Equipment costs $149.99 to $349.99, depending on your package. However, keep in mind that you will need to purchase the equipment upfront, which will cost you between $100 and $350 — not exactly cheap. But still, we think Aloe Care Health is a great option for seniors who could use a little extra care and coverage.
| Connectivity | Cellular |
|---|---|
| Fall Detection | Included in some plans |
| In-home Range | 200 feet |
| Battery Backup | Yes |
| GPS Option | Yes |
| Money-back Guarantee | 30-day |
Our senior care experts personally test, review, and recommend systems that are the best in their category. Everything we publish is 100% unbiased and objective.
And we would never recommend products that we don’t truly believe in. This means you get an expert in your corner to guide you and help you find an alert system that makes sense for your budget and lifestyle.
Our goal is to remain a top resource that helps seniors live more independently with peace of mind. And we can only accomplish this if readers like you trust our integrity and ethics. So we always strive to remain:
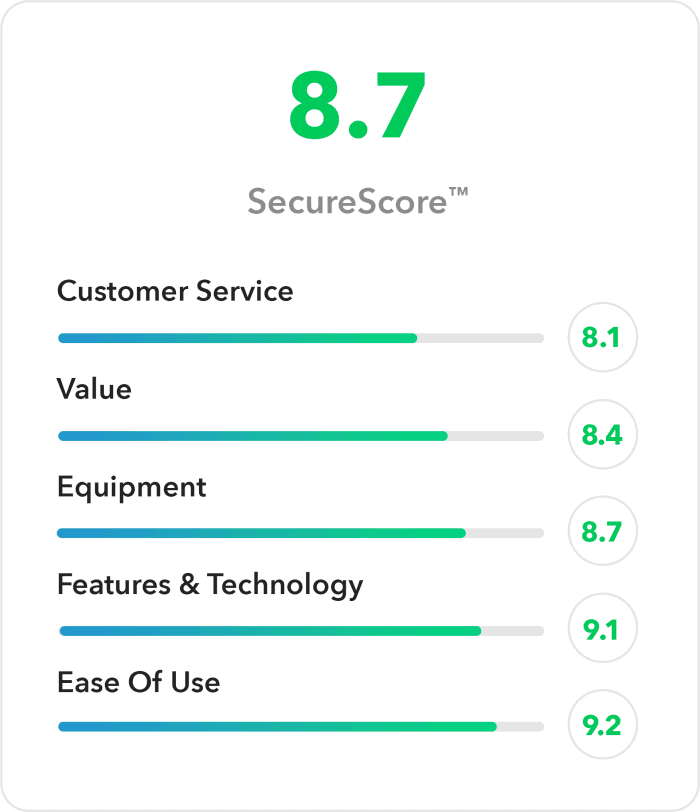
Our SecureScore™ rating system
You might already know that our research and testing results in our proprietary SecureScore™. This score covers 5 important categories: Customer Service, Value, Equipment, Features and Technology, and Ease of Use. In other words, we do our best to get a full understanding of what it’s like to actually use the best alert systems on a daily basis. Then we share our findings with you! We do the homework so that you don’t have to.
It’s no secret that there are lots of medical alert systems to choose from. But narrowing down your options and making a decision doesn’t have to be complicated. In fact, it should be easy! That said, you’ll want to look out for little things that can turn into big-time deal-breakers.
For instance, not all help buttons are waterproof (there goes safe showering!). And did you know that some only have a 300 ft. range from the base station, while others work up to 1,300 ft. or more. Also, certain alert systems only work at home, while others work on-the-go. Don’t worry — we’re going to show you exactly what to look for in a medical alert system.
FYI: Most slip and falls happen in the bathroom, that’s why we always recommend a waterproof alert system. With a waterproof device, you or your loved one can bathe or shower without sacrificing safety.
As they say, you don’t know what you don’t know! That’s why you have us. We’re going to cover features and monitoring, monthly costs and fees, customer service, and other important points you should keep in mind. So let’s dive right in.
Now, you might be tempted to go straight to the top-rated alert system on the market, place your order, and call it a day. But that could be a mistake. Why? While Bay Alarm Medical and Medical Guardian are ranked #1 and #2 on our list, you should know that each brand out there sells a handful of different devices, each meant for totally different lifestyles.
The truth is, whether the system is for you, or a loved one, which medical alert system is the best depends on how you will use it. Think about activity level and lifestyle: will it mostly be used at home? Or is the user active and out and about a lot? If you love to visit friends, go shopping and lead an active lifestyle, a mobile system like a smartwatch is recommended. But if you spend the majority of time at home, an in-home alert system is the better choice.
FYI: If you or a loved one lives with diabetes, there are a few unique features to look out for when shopping for an alert system. Learn all about it in our guide to the best medical alert devices for diabetics. It’s important to do your research up front, especially since some brands charge high prices for what you get. In our research, we found that while Life Alert’s GPS systems might work for diabetics, Life Alert costs are pretty high.
In-Home Alert Systems – A pendant alert will summon emergency response help at the push of the button. Note that the biggest advantage of in-home systems is their affordability: they range between $24.99 to $39.99 per month. But their main weakness is their short range. Some will keep you protected while you’re in your house and gardening out back, but you won’t have coverage when you leave home. So that’s something to keep in mind.
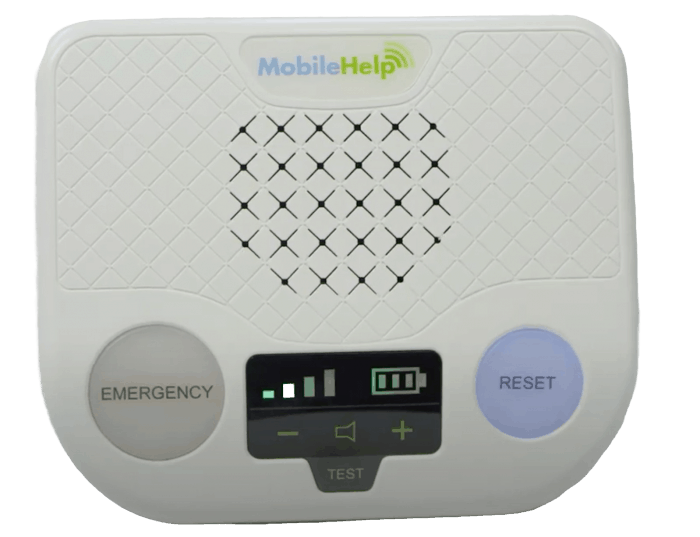
MobileHelp In-Home Medical Alert Base Station
Pro Tip: In-home or mobile alert? It’s the age-old question. And it’s the primary difference between alert systems. If you can swing the extra cost, we recommend choosing a mobile unit, especially if you or your loved one lives an active lifestyle.
Mobile Alert Systems – We think these are great for active older adults who want emergency coverage on-the-go. Instead of running off your home Wi-Fi network or landline, mobile medical alerts are powered by reliable cellular signals (just like modern smartphones!). This means you can go pretty much anywhere in the country, so long as there’s a cell signal. You can choose from bracelets, necklace pendants, and even fashion-forward smartwatches.

Lively Wearable 2 and Mobile Plus
One nice feature of some mobile alert systems is GPS location tracking. This allows emergency personnel to quickly locate your whereabouts when it matters most. If you have an elderly parent who is prone to getting lost or disoriented, you’ll probably want a mobile alert with GPS. We think you'll like the unlimited nationwide range. Just keep in mind, they cost more than at-home alert systems.
Thankfully, it only takes a few minutes to set up an alert system. Most brands offer plug-and-play setup these days. If you have an in-home unit, you’ll plug the base station into your wall and follow the step-by-step prompts. Mobile units are even easier to get started. So even if you’re not Bob Vila with lots of DIY handy skills, you should have no issues. That said, some seniors choose to have their tech-savvy children set it up for good measure.
These devices are meant to save your life during a health crisis or other emergency. Every second matters, so you can imagine that the products are easy to use (actually, they’re foolproof!). And if it’s not easy to use, you won’t find it anywhere on our site.
No matter the time of day or night, all you have to do is press the help button and your alert sends a signal to a professional monitoring center. The monitoring center fields the alert, typically within 15 to 30 seconds, and they jump into action to get you the help you need. They can call police, fire, or EMS. Alternatively, they can call a friend or family member to check on you.
Did You Know? One of our top-rated medical alert systems, Medical Alert, has an average response time of under 20 seconds.
Something else to consider when deciding on the best alert device for you is the ability to communicate two ways. This is an important feature to look out for, because with a built-in speaker and microphone, you or your loved one can speak with emergency personnel directly, through either a base station or a wearable unit. Again, we’ve found the vast majority of systems are user friendly and easy to use–but some are easier than others!

LifeStation Mobile LTE Medial Alert
When you’re researching at-home medical alert systems, you’ll notice that many offer either a landline or cellular connection. So what’s the difference? Well, the difference is night and day. We recommend a system that works best for you in communicating with the monitoring center so that you can get help immediately. Remember, seconds matter when it comes to an emergency.
With this in mind, landline alerts tend to be a bit slower, but they are also the cheapest. Cellular systems can be quicker. However, they use the provider’s cellular connection. Choose a cellular system only if you receive a strong signal in the area that you live.
While some brands require upfront payment for equipment, you’ll like that today’s best alert companies include the equipment for free with paid monitoring. So it’s usually pretty cheap to get started. Depending on the type of system you choose, you should expect to pay between $19.99 and $49.99 per month for potentially life-saving emergency coverage. Here’s a basic rundown of monitoring costs:
Some companies, like Life Alert, require miscellaneous fees like membership fees and activation fees. Of course, we’d rather not pay these additional costs, but sometimes it’s worth it. We recommend finding a system that doesn’t charge extra fees (and there are lots out there!). But if you do have to fork out a little more money to get started, just be sure it’s under $100.
We think a company that charges a dime more than $100 just to get started probably cares more about making money than helping seniors. So steer clear of those guys! Thankfully you can get the coverage you need without breaking the bank. Aim to keep your first bill (and subsequent bills) under $40-$50, even with fall detection.

MobileHelp Fall Detection Neck Pendant
Fall detection is a popular add-on that we’ve tested extensively. It’s usually built into an alert device, and it automatically signals the monitoring center when it detects a slip or fall. Note that most alert companies charge a flat fee of $10 per month for fall detection. But keep an eye out for $5 monthly fall detection — as top brands like LifeFone offer it on-the-cheap.
FYI: Fall detection isn't 100% accurate, but we still recommend getting this life-saving upgrade. Falls are the leading cause of injury-related death among adults age 65 and older.1 For an extra $10 a month, your alert system can call for emergency help, even if you're unable to.
You can also buy add-ons like a key lockbox to give first responders access to your home during an emergency ($29-$49), a Vial of Life to share your medical history and medications with first responders ($10), and extra help buttons for around your home ($10-$20). We advise you to go easy on the add-ons and upgrades, as you can always buy them as needed in the future.
When it comes to staying on the cutting edge and continuing to innovate in new and exciting ways, we’ve found there are just a handful of medical alert companies that are above the fray. Bay Alarm Medical, Medical Guardian, and Lively are three companies that are constantly introducing new technology and making advancements in senior safety.
While our list below of the latest (and greatest!) technology isn’t 100% exhaustive, it does cover the main advances in the medical alert industry as of late. Of course, the features and tech will continue to evolve over the years, as competition is sure to drive innovation. Thankfully it’s a win-win situation for seniors and caregivers alike. Here are a few of our favorite alert features.
| Feature | How It Works |
|---|---|
| Automatic Fall Detection | Fall detection uses the same electromechanical technology that airbags use to save lives. With a combination of accelerometers, sensors, and sophisticated algorithms, fall detection devices measure acceleration and changes in velocity. If the system senses a sudden change in speed or velocity, the alert system automatically contacts the monitoring center on your behalf. |
| GPS Location Services | GPS (or Global Positioning System) uses 30 satellites that orbit 12,500 miles above the Earth’s surface! Now, if you happen to slip and fall while out for a walk, your alert system with GPS will triangulate your exact location using those satellites. This allows a caregiver or emergency responders to find you in a jiffy. Many mobile cellular systems offer this. |
| Two-Way Communication | The top medical alert systems offer two-way communication, which can save a life in the event of a fall or other emergency. We’ve found that Bay Alarm Medical has one of the best two-way talk features in the industry. The high-output speakers and sensitive microphones allow you to talk with the monitoring center when it matters most. It’s especially helpful for seniors who lack mobility. |
| 5G LTE Connection | We've found that 5G LTE cellular technology offers the fastest results. You don’t need a landline to use it, and the upgrade is typically cheaper than installing a landline in your home. Just expect to pay an extra $5 to $10 per month for it. |
| Mobile App / Caregiver Tools | We think you’ll like that select alert systems let you track your loved one’s whereabouts using a modern mobile app. Other than location monitoring (using that neat GPS feature we talked about), you can review activity reports, use two-way talk, receive event notifications, etc. So if you’re looking for a little extra peace of mind, we recommend checking out the Caregiver Connection offered by Bay Alarm Medical or Philips Cares from Lifeline. |
| Fast Response Times | This doesn’t point to any specific technology, it’s more of a nod to the monitoring centers. A handful of alert systems (see our top 10 list above) are backed by CSAA Five Diamond monitoring centers. These centers are staffed with highly-trained emergency responders. Most offer response times under 30 seconds, with others clocking in closer to 10-15 seconds. Now that’s fast! |
| Environmental Monitoring | Older adults are at higher risk for fire-related deaths. Thankfully, we've used a handful of medical alert systems that offer reliable environmental monitoring as an upgrade. You'll pay a little extra for the sensors, and maybe $10 more per month for monitoring, but we think it's worth the cost. |
| Languages Supported | English not your native language? You’re in good hands, as the best medical alert companies now support over one hundred different languages. So long as you choose a company like ADT Health that provides multilingual support, you’ll get the response and care you deserve no matter the language you speak. |
FYI: Many medical alert devices use Bluetooth to ensure a reliable connection.
Very few companies require lengthy contracts these days, and most don’t require any contract at all. That’s really good news. The way we see it, aging is an uncertain new stage of life, and companies should offer flexibility in their terms and conditions. So keep in mind there’s no need to sign a contract, as there are loads of top quality medical alert systems that offer affordable month-to-month deals.
That said, you can sometimes save money by signing up for longer-term contracts. Many companies, like Bay Alarm, offer discounts when you commit to quarterly or annual plans.
You’ll also want to look for other customer-friendly policies like money-back guarantees, free activation, free shipping, and the like. The truth is, alert systems are becoming more popular every day, so companies are scrambling to secure their share of the market — which means deals and discounts for folks like you!
We offered information on Medicare coverage in bite-sized pieces above. You may be thinking: doesn’t this cover everyone using medical devices? The vast majority of individuals who use or might benefit from using a medical alert device receive their medical benefits through some form of Medicare. But not everyone. Below are a few other groups of people who might be seeking coverage for medical alert devices.
(One other group not yet mentioned are individuals using Veteran’s benefits. We will discuss these benefits in more detail below.)
The three groups of individuals mentioned above use either job-based insurance plans, plans bought directly from insurance companies or plans purchased through the “marketplace” set up by the Affordable Care Act (ACA).
We have noticed that health insurance plans are covering more and more preventative services than they have done in years past. So whether private insurance companies completely cover or discount medical alert devices is a great question to ask. Unfortunately, the answer for most insurance companies is no, medical alert devices are not covered by insurance. We do recommend contacting your provider to learn about the specifics in your policy.
From our research, the Veteran’s Administration (VA) partners with two medical alert providers to offer specific devices free to eligible veterans. Here’s the breakdown:
LiveLife Mobile Alarm offers a wearable pendant worn around the neck. It can text or call designated contacts, including 911, and uses a 4GX network for two-way talk and location tracking. However, it does not connect to a certified 24/7 monitoring center, a feature most other systems include. It does offer fall detection, which we consider essential.
MedEquip Alert provides a necklace or belt-clip device that runs on LTE, allowing use both at home and on the go. It includes two-way talk with a 24/7 monitoring center and GPS tracking, but lacks fall detection.
While each device misses one or two features compared to other systems, we appreciate that the VA provides a baseline of protection for older veterans. Full insurance coverage for medical alert devices is rare, so this is a valuable benefit. Veterans also have the option to choose a more comprehensive system, with partial coverage provided through VA Medical Health Care.
There are some products you simply can’t take chances with, and medical alert systems are at the top of that list. You’re investing in a device and monitoring plan that could save your life, so it’s crucial to choose a company you trust and a system you feel confident using.
Every system has its strengths and trade-offs. Some focus on advanced features, others on affordability. Some excel in mobile alerts, while others shine with in-home coverage. One thing we can guarantee from our years of testing: every system on this list is reliable and designed to keep you safe. Take your time—review the options, revisit this list when you have a system in mind, and compare features carefully. Our goal is to help you choose a system that truly protects you and fits your needs.
It depends. We typically recommend fall detection for seniors who are prone to slip and falls, like seniors with balance problems, bone & joint issues, diabetes, vision loss, and the like. If you or your loved one is still active at home (and away from home), fall detection might not be necessary. But it’s an individual choice that you have to make. The good news is that it typically only costs an extra $5 to $15 per month, which we find well worth it.
You should certainly consider an alert system for your spouse or partner. After all, if you two aren’t together if/when an emergency occurs, one of you will get the short end of the deal. The good news is that most medical alert companies offer coverage for a spouse or other household occupant at a greatly reduced price. Sometimes they’ll even offer additional coverage for free. So in our eyes, there’s no reason to forego coverage for your spouse or partner.
As experts, we always recommend a full-on waterproof alert device. We mentioned before that most falls happen in the bathtub or shower, so you should think of the bathroom as a hot-spot for medical emergencies. Now, if you go with a water-resistant pendant (or another wearable), it won’t function when submerged or exposed to heavy water use. A waterproof help button, on the other hand, will keep you protected even when submerged. So it’s easy to see the advantage of waterproof alert systems. That said, it’s best to check with the manufacturer to clarify the capabilities of their medical devices before deciding on which one is right for you.
Unfortunately, no they aren’t covered by Medicare at this time. Since Medicare does not consider these devices as a “medical necessity,” they typically are not covered by Medicare Parts A and B. Obviously, the majority of seniors and leaders in the medical alert industry (including us!) argue that alert systems are absolutely a medical necessity. But don’t expect your Medicare plan to cover your monthly monitoring fee. With that said, in some cases, Medicare Part C does cover alerts. It’s also worth noting that certain healthcare reimbursement accounts (HSA’s) cover alert devices as well.
That’s an easy one to answer! We recommend you get an at-home system if you (or your loved one) spends the majority of your time at home. However, if you live a more active lifestyle and leave home often, we recommend getting a cellular mobile alert system.
Center for Disease Control. (2024). Older Adult Falls Data. https://www.cdc.gov/falls/data-research/index.html
Library of Congress. (Accessed July 19, 2020). What is a GPS? How does it work? https://www.loc.gov/everyday-mysteries/item/what-is-gps-how-does-it-work/
LTE Telecommunication. Wikipedia. (Retrieved July 20, 2020). https://en.wikipedia.org/wiki/LTE_(telecommunication)
National Institute of Standards and Technology (NIST). Butry, D.T; et. al. (2017, August 22). NIST Study Suggests Frailty Makes Elderly More Likely to Die in Home Fires. https://www.nist.gov/news-events/news/2017/08/nist-study-suggests-frailty-makes-elderly-more-likely-die-home-fires